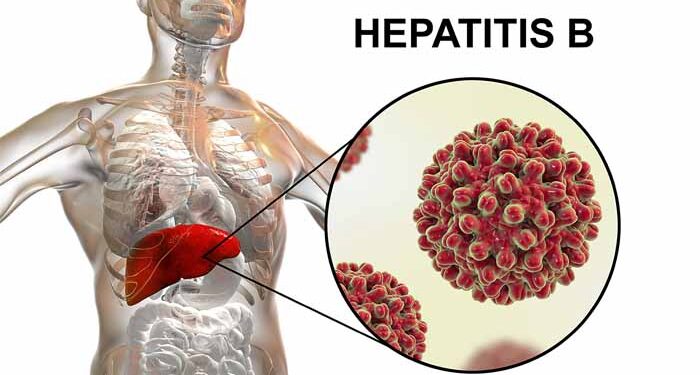
- Hepatitis B is a viral infection that affects the liver.
- Despite the availability of a safe and effective vaccine, large pockets of the population remain vulnerable—either due to missed childhood immunisations, lack of awareness, or low-risk perception
- According to the estimates by the World Health Organization, around 3–4% of the Indian population is chronically infected
- Young people who are not sure of their vaccination history can benefit from serological screening, followed by a three-dose vaccine series if needed
DR SANDEEP KUMBAR

Hepatitis B is often overshadowed by better-known infections, yet it remains one of the most serious public health threats, worldwide. In India, the disease continues to circulate silently, particularly among young adults. Despite the availability of a safe and effective vaccine, large pockets of the population remain vulnerable—either due to missed childhood immunisations, lack of awareness, or low-risk perception. The result is quiet but a persistent reservoir of infection that continues to threaten long-term liver health.
Hepatitis B is a viral infection that affects the liver. Known to be caused by hepatitis B virus (HBV), which can lead to both acute and chronic illness. Chronic hepatitis B can result in liver fibrosis, cirrhosis, or even liver cancer over time. HBV major concern is that it can be transmitted through blood, unprotected sexual contact, or from mother to child during birth—routes that are not always recognised as high-risk among young people.
India is considered a country of intermediate endemicity for hepatitis B. According to the estimates by the World Health Organization, around 3–4% of the Indian population is chronically infected. Many of those living with HBV are unaware of their status. The infection can remain asymptomatic for years, it often goes undetected until significant liver damage has already occurred. For young adults, the delay in diagnosis can have lifelong implications.
While hepatitis B vaccination has been included in India’s Universal Immunisation Programme since 2002, implementation gaps persist. Those born before this period or in regions with limited healthcare access may have missed vaccination entirely. There is also a lack of routine catch-up programmes for adolescents or young adults who were never vaccinated as infants. In places where young people live in close quarters or are sexually active—the risks multiply when vaccination coverage is incomplete.
The challenge is compounded by a widespread lack of understanding about the disease. Many associate hepatitis solely with food or water contamination, which actually pertains more to hepatitis A and E. Hepatitis B, in contrast, is a bloodborne infection. Sharing razors, dental equipment, tattoo needles, or even undergoing minor medical procedures in unregulated settings can all serve as potential modes of transmission. Among sexually active youth, low condom sexual activity with multiple partners can increase the vulnerability to this infection, especially in the absence of vaccination.
In the context of India’s rising burden of liver diseases, overlooking hepatitis B prevention in young adults could have long-term consequences. Chronic infection acquired in adolescence or early adulthood quietly damages the liver over decades. By the time symptoms surface—often in the form of fatigue, jaundice, or abdominal swelling—the liver may already be severely compromised. Treatment is available but lifelong for many, and access to consistent monitoring is not always assured in lower-resource settings.
Timely diagnosis is key. A simple blood test can identify HBV infection or confirm immunity. Young people who are not sure of their vaccination history can benefit from serological screening, followed by a three-dose vaccine series if needed. The vaccine is over 95% effective in preventing infection and offers long-term protection. Yet, uptake remains low outside paediatric care settings.
Preventive healthcare often takes a backseat in the twenties and early thirties—a time when individuals feel least vulnerable to chronic illness. But this is precisely the window when protection can be most effective. Public health messaging around hepatitis B should reach beyond childhood immunisation and actively target young adults—especially those in colleges, vocational training institutes, and early employment stages.
Addressing hepatitis B requires a shift in how risk is communicated. Rather than waiting for liver symptoms to appear, the focus must move toward early awareness, voluntary screening, and proactive vaccination. These steps are not only medically sound but also cost-effective public health measures that prevent long-term complications.
In a generation that routinely takes charge of its career, relationships, and digital security, taking charge of health should be no different. A simple vaccine today can safeguard decades of liver health tomorrow. For Indian youth, protection begins with information—and the decision to act on it.
The author of this article is Dr Sandeep Kumbar, Consultant Medical Gastroenterologist, Hepatologist & Therapeutic Endoscopist, HCG Suchirayu Hospital, Hubli.